needs and therefore becomes stored as fat.
Gestational Diabetes Causes, Symptoms, and Consequences
Causes of gestational diabetes during pregnancy can be effected by previous health issues. Women who are overweight, have had gestational diabetes before, or have an immediate family member with type 2 diabetes, could be more susceptible of getting diagnosed with gestational diabetes. By losing extra weight and increasing physical activity before and during pregnancy, you will greatly minimize any chances of getting gestational diabetes.
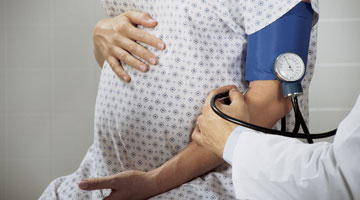
Barbara J. Moore, PhD and health expert discusses one of the key causes of pregnancy health issues. “We know for example that obese pregnant moms are at high risk for gestational diabetes, which is pregnancy diabetes, or gestational hypertensions, which is pregnancy high blood pressure. So it shouldn’t be surprising that obesity is also affecting the developing baby,” she shares about how being overweight can affect your pregnancy and child.
Babies born to mother’s with gestational diabetes are at higher risk for breathing problems, obesity and diabetes. If untreated, babies can be born with a larger than normal body which makes the delivery process difficult and dangerous. Further consequences of gestational diabetes include: low blood glucose levels, respiratory distress, and jaundice.
“One of the main complications is that the baby can grow to be too big and that can lead to difficulty at the time of delivery, with the shoulders becoming entrapped and sometimes damage to the nerves of the neck or arms,” says Chief of Maternal Fetal Medicine at Children’s Hospital LA, Dr. David Miller. “Babies who are born to women who have diabetes sometimes have difficulty with their own sugar control after they are born,” he continues.
Gestational diabetes will not only effect the baby, but the mother as well. Women who experience gestational diabetes during their pregnancies are more likely to have symptoms of preeclampsia, need a C-section at birth, or become depressed. The development of type 2 diabetes has also been linked to having gestational diabetes during pregnancy. Regular communication with your doctor and maintenance of a healthy lifestyle will decrease chances of these symptoms.
After pregnancy, gestational diabetes usually goes away. Once you have experienced gestational diabetes during one pregnancy, the chances that it will return in future pregnancies are higher. Lifestyle and diet changes after pregnancy can prevent against the later development of type 2 diabetes.
Gestational Diabetes Diet
A wholesome diet is vitally important for pregnant women, especially those diagnosed with gestational diabetes. Healthy proportions of the right kind of food can be one of the best ways to control any symptoms for you or your unborn baby. Vegetables, fruits, proteins, and whole grains are all great examples of foods that have high nutrition levels and low fat and caloric levels.
It is important to consult a registered dietitian or diabetes expert for further education, since no single diet will work for everyone. Creating a plan and menu for meals and snacks during the day is a great way to monitor what you are eating. Dietitians can also recommend recipes for breakfast, lunch, and dinner to help facilitate a nutritious diet.
Nutritionist and expert Del Millers, PhD explains, “You don’t want to eat things that are going to go right into the blood stream and cause you to have a sugar high, because again your body cannot use the insulin that it’s producing, so all that sugar is going to remain in the blood stream and possibly get into the placenta.”
Gestational Diabetes Treatment
To prevent severe damages to you and your baby, find treatment solutions that will work for you. Specific, regimented meal plans and plenty of physical activity are helpful ways to lower blood glucose levels. As well, insulin injections and blood glucose testing could be suggested by a physician or health-care provider to monitor symptoms.
The American Diabetes Association published the following guidelines for women who are testing their blood glucose levels. The measurement of milligrams per deciliter represents the concentration of a certain substance in the given amount of fluid. In this case, the amount of glucose in the bloodstream is tested.
Before a meal (preprandial): 95mg/dl or less
1- hour after a meal (postprandial): 140 mg/dl or less
2-hours after a meal (postprandial): 120 mg/dl or less
Normal checkups with your doctor after giving birth are very important in maintaining the health of you and your baby. If necessary, your doctor could prescribe you with oral medication or insulin injections.
However, gestational diabetes is not a permanent condition, so make sure to take care of yourself and live a healthy and active lifestyle
Our experts:
Del Millers, PhD
David Miller, MD
Ling Wong, MS, CHC
Anthony Chin, MD
Barbara J. Moore, PhD